
Md. Al Foyjul Islam
Received: 2022-11-11 | Revised:2022-11-27 | Accepted: 2022-11-28 | Published: 2022-12-05
Abstract
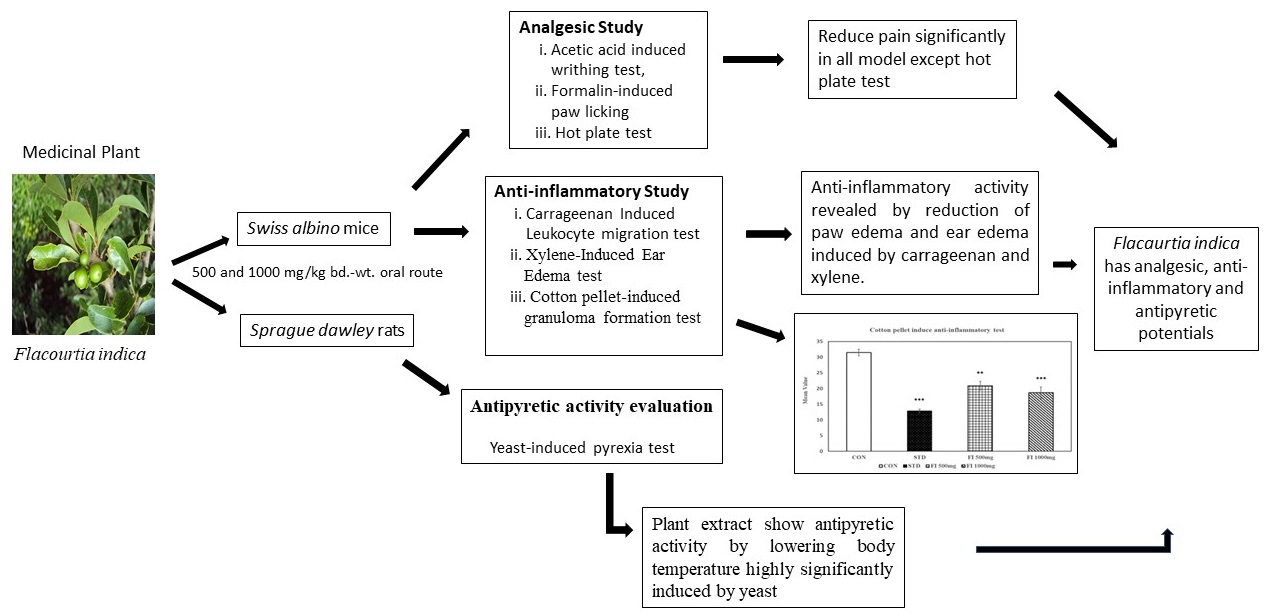
Worldwide attention on plant study has
expanded, and a wealth of data has accumulated to demonstrate the enormous
potential of medicinal plants employed in diverse traditional systems. In the
traditional medical system, Flacourtia indica (FI) has been used to cure
a variety of illnesses, including cancer, diabetes, hepatic disorders, and
snakebites. Due to the presence of a variety of
phytochemicals, including alkaloids, flavonoids, tannins, terpenoids,
glycosides, it may have antioxidant and anti-inflammatory activity. Thus, this
study was designed to assess the analgesic, anti-inflammatory and antipyretic
effects of the ethanolic extract of Flacourtia indica. Flacourtia indica was extracted using 100% ethanol
followed by assessing acute
toxicity
and doses selected for the studies were 500 and 1000 mg/kg body weight. Swiss albino mice of either sex weighing 25-30 gm and Sprague dawley
rats weighing 180-200 gm were used in
this study. Analgesic activity was evaluated by using acetic acid
induced writhing test, formalin induced paw licking and hot plate test.
Anti-inflammatory effect was assessed using xylene and croton oil induced ear
edema test and carrageenan induced paw edema test. Also the antipyretic effect
was investigated. The
Flacourtia indica extract exhibited significant effect against pain in
acetic acid test (p<0.01), formalin test (p<0.01) and insignificantly in
hot plate test. Inflammation was reduced by FI extract in xylene test
(p<0.05), croton oil test (p<0.01) and significantly reduced the paw
edema (p<0.001) in carrageenan-induced paw edema test. In the yeast-induced
antipyretic test, administration of Flacourtia indica at both doses
significantly (p< 0.001) reduced pyrexia. Within
these two doses, higher doses (1000 mg/kg body weight) had better aptitudes in
the reduction of pain, inflammation and pyrexia. The FI extract shown
strong analgesic, anti-inflammatory, and antipyretic capabilities, according to
the study results, and more research is needed to assess these effects and the
potential of the plants.
Keywords:
Medicinal plant, Flacourtia
Indica, analgesic effect, anti-inflammatory effect, yeast
induced pyrexia.
References
1. Thirunethiran, K.; Varalakshmi,
B.; Suguna Bai, J.; Gomathi, S. Effect
of different doses of cucurbita pepo linn extract as an anti-inflammatory and
analgesic nutraceautical agent on inflamed rats. Int.
J. Phar. Res. Dev, 2011, 3(7), 60-78.
2. Estakhr, J.; Sanchooli, N.; Najafi,
S.H.; Javdan, N. Anti-Inflammatory Activity of Ethanolic Extract of Physalis
alkekengi. Res. J. Pharm. Biol. Chem. Sci. 2011, 2(3),
421-425.
3. Wohlmuth, H.; Oliver, C.; Nathan,
P.J. A review of the status of Western herbal medicine in Australia. J.
Herb. Pharmacother, 2002, 2, 33-46.
4. http://www.floraofbangladesh.com/2020/05/boichi-or-madagascar-plum-flacourtia.html.
5. Eramma, N.K. A Comprehensive Review
on Pharmacology of Flacourtia Indica (BURM.F.) Merr. (governor’s Plum). Int.
J. Pharm. Chem. Sci. 2016, 5(3).
6. Kirtikar, K.R.; Basu, B.D. Indian
Medicinal Plants. 3rd ed. Vol II, Singh and MP Singh Publications. India. 1998,
220.
7. Kaou, A.M.; Leddet, V.M.; Canlet.
C.; Debrauwer, L.; Hutterm, S. Antimalarial compounds from aerial parts of
Flacourtia indica (Flacoutiaceae). J Ethnopharmacol. 2010,
130(2), 272-274.
8. Pachute, P.A.; Tyagi, S.; Mishra,
A.; Shakya, A.; Kumar, D.; Patel, V.K. Preliminary evaluation of Anticancer
activity of Flacourtia indica Merr. Bot. Res. Int. 2011,
4(3),43-47
9. Asad, B.H.H.M.; Murtaza, G.; Siraj,
S.; Khan, A.S.; Azhar, S.; Hussain, S.M.; Ismail, T.; Hussain, S.M.; Hussain,
I. Enlisting the scientifically unnoticed medicinal plants of Pakistan as a
source of novel therapeutic agents showing anti-venom activity. Afr. J.
Pharma. Pharmacol. 2011, 5(20), 2292-2305.
10. Kim, J.S.; Ju, J.B.; Choi, C.W.;
Kim, S.C.; Hypoglycemic and antihyperlipidemic effect of four Korean Medicinal
plants in alloxan induced diabetes rats. Amer. J. Biochem. Biotech. 2006,
2(4), 154-160.
11. Koster, R.; Anderson, M.; De-Beer,
E.J. Acetic acid analgesic screening. Fed. Proc. 1959, 18,
412–417.
12.
Eddy,
N.B.; Leimbach,
D.
Synthetic Analgesics II. Dithienylbutenyl- And Dithienylbutylamines. J. Pharmacol.
Exp. Therap. 1953, 107(3), 385-93.
13. Hunskaar, S.; Hole, K. The formalin
test in mice: dissociation between inflammatory and non-inflammatory pain. Pain
1987, 30, 103-114.
14. Vinegar,
R.; Schreiber, W.; Hugo R, Biphasic development of carrageenan-induced oedema
in rats. J. Pharmacol. Exp. Ther. 1969, 166, 96-103.
15. Dai, Y.; Liu, L.H.; Kou, J.P.;
Anti-inflammatory effect of aqueous extract of Wu-HU-Tang. China. Pharm.
Uni. 1995, 6, 362-364.
16. Swingle, K.F.; Shideman, F.E.
Phases of the inflammatory response to subcutaneous implantation of a cotton
pellet and their modification by certain anti-inflammatory agents. J.
Pharmacol. Exp. Ther. 1972, 185, 226–234.
17. Loux,
J.J.; De Palma, P.D.; Yankell, S.L. Antipyretic testing of aspirin in rats. Toxicol.
Appl. Pharmacol. 1972, 22, 672–675.
18. Victor, B.O.; Caleb, O.W.; Ayodele,
O. S.; Samuel, B.O. J. Ethnopharmacol. 2004, 90, 317-321.
19. Vyklicky, L.Techniques for the
study of pain in animals, In: Bonica, J.J.; Liebeskin &
Albe-Fessard, D.G. (Eds), Advances in Pain Research and Therapy. Raven. New
York, USA, 1979, 773-778.
20. Vongtau, H.O.; Abbah, J.; Mosugu,
O., et al. Antinociceptive profile of the ethanolic extract of Neorautanenia
mitis root in rats and mice. J. ethnopharmacol. 2004, 92(2-3),
317- 324.
21. Tjolsen, A.; Gerge, O.G.; Hunskaar,
S., et al. The formalin test: an evaluation of method. Pain 1992, 51,
3-17.
22. Ghannadi, A.; Hajhashemi, V.;
Jafarabadi, H. An investigation of the analgesic and anti-inflammatory effects
of Nigella sativa seed polyphenols. J. Medicinal. Food. 2005,
8, 488-493.
23. Gabor, M. Mouse
Ear Inflammation Models and their Pharmacological Applications. 2000,
Akadémiai Kiadó, Budapest, Hungary.
24. Halliwell, B.; Gutteridge, J.M.C.
Free radicals in biology and medicine, 1999, Oxford University press.
25. Conner, E.M.; Grisham, M.B. Inflammation, free radicals, and antioxidants.
Nutrition 1996, 12(4), 274-277.
26. Collier, H.O.; Dinneen, L.C.; Johnson, C.A.; Schneider, C.
The
abdominal constriction response and its suppression by analgesic drugs in the
mouse. Br. J. Pharmacol. 1968, 32(2),
295–310.
27.
Deraedt, R.; Jouquey, S.; Delevallée, F.; Flahaut, M. Release of prostaglandins E and F in an algogenic reaction and
its inhibition. Eur. J. Pharmacol. 1980, 61(1), 17-24.
28. Roberts, L.J.; Morrow, J.D.
Analgesic, antipyretic and Anti-inflammatory Agents and Drugs Employed in the
Treatment of Gout. In: Eds. Goodman and Gilman’s The Pharmacological Basis of
Therapeutics. 10th ed., McGraw-Hill. New York; 2001, 687-732.
29.
Richardson, Kilo Hargreaves Cannabinoids reduce hyperalgesia and inflammation via
interaction with peripheral CB1 receptors. Pain 1998, 75(1),111-119.
30. Bensreti, M.M.; Sewell, R.D.E.
Selective effects of dopaminergic modifiers on antinociception produced by
different opioid receptoragonists. Pro. Br. Pharmacol. Soc. 1983,
6th – 8th July,70.
31. Headley, P.M.; O’Shaughnessy, C.T.
Evidence for opiate and dopamine interaction in striatum. Br. J. Pharmacol.
1985, 86 (pro. Suppl.), 700.
32. Wigdor, S.; Wilcox, G.L. Central
and systemic morphine-induced antinociception in mice: Contribution of
descending serotonergic and noradrenergic pathways. J. Pharmacol. Exp. Ther.
1987, 242, 90-95.
33. Pasero, C.; Paice, J.A.; McCaffery,
M. Basic Mechanisms underlying the causes and effects of pain. In Pain,
McCaffery M, Pasero C (eds). Mosby: St. Louis 1999, 15- 34.
34. Salvemini, D.; Wang, Z.-Q.; David, M.B.; Michael, K.S.; Mark, G.C.; Pamela, T.M.
Evidence of peroxynitrite involvement in the carrageenan-induced rat paw edema.
Eur. J. Pharmacol. 1996, 303(3), 217-220.
35.
Loram, L.C.; Fuller, A.;
Fick,
L.G.; Cartmell, T.; Poole, S.; Mitchell,
D. Cytokine Profiles During Carrageenan-Induced
Inflammatory Hyperalgesia in Rat Muscle and Hind Paw. J. Pain 2007,
8, 127-136.
36. Ribeiro, R.V.; Matos da Silva, R.;
Joaquim Lima, J.C.S.; Martins, D.T.O. Antiinflammatory, antinociceptive and
antipyretic effects of hydroethanolic extract from Macrosiphonia velame (A.
St.-Hil.) M. Arg. in animal models. Braz. J. Pharm. Sci. 2010,
46(3), 515-523.
37. DiMartino, M.J.;
Campbell, J.R.G.K.; Wolff, C.E.; Hanna, N.; The pharmacology of arachidonic
acid-induced rat paw edema. Agents and Actions 1987, 21 (3-4),
303-305.
38. Luber-Narod, J.; Austin-Ritchie,
T.; Hollins, C.; Menon, M.; Malhotra, R.K.; Baker, S.; et al. Urol. Res.
1997, 25, 395–9.
39. Atta, A.H.; Alkofahi, A.
Anti-nociceptive and anti-inflammatory effects of some Jordanian medical plant
extracts. J. Ethnopharm. 1998, 60,117-124.
40. Kavimani, S.; Vetrichelvan, T.;
Ilango, R.; Jaykar, B. Antiinflammatory activity of the volatile oil of Toddalia asiatica. Indian. J. Pharm. Sci.
1996, 58(2), 67–70.
41. Simmons, D.L.; Botting, R.M.; Hla,
T. Cyclooxygenase isozymes: the biology of prostaglandin synthesis and
inhibition. Pharmacol. Rev. 2004, 56, 387-437.
This work is licensed under the Creative Commons Attribution 4.0 License (CC BY-NC 4.0).